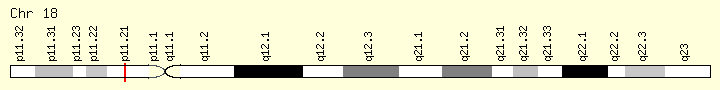This web page was produced as an assignment for Genetics 564, an undergraduate course at UW-Madison. http://genetics564.weebly.com/
What is Crohn's disease?
Crohn’s disease is a an autoimmune disease that affects the GI tract. The autoimmune reaction results in massive inflammation in the GI tract and causes chronic diarrhea, fever, abdominal cramping, reduced appetite, weight loss, and bloody stool. Severe cases will need surgery to remove the affected part of the intestine and will be replaced with a colostomy bag that needs to be emptied throughout the day. These symptoms make life extremely difficult for those who have Crohn's disease and with no known cure, they are fated to deal with the symptoms for the rest of their life.
Crohn's disease affects over 700,000 Americans and if not managed properly, those affected are fated to live a life of discomfort and pain.
Crohn's disease affects over 700,000 Americans and if not managed properly, those affected are fated to live a life of discomfort and pain.
What is an autoimmune disease?
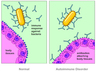
An autoimmune disease occurs when your body begins to recognize its' own cells as foreign and subsequently attacks itself. The immune system's role is to protect against infection by killing foreign cells in your body via antibody recognition. In an autoimmune disease there is a disruption in this system and the body begins to attack itself.
Crohn's Disease Videos:
|
|
|
|
What causes Crohn's disease?
The exact cause of Crohn’s disease is unknown. However, environmental stressors and genetic links have been associated with disease onset.
ENVIRONMENT
Environmental factors such as stressful life events [1], air
pollution [2], a Western diet [3], and smoking [4-6] all
have been associated with Crohn’s disease and can potentially lead to an
increased risk for the disease [7].
GENETICS
Genes involved in the immune response have been identified as possible risk factors. Many genes have had close links with disease susceptibility. The most heavily studied gene is NOD2 which regulates inflammation in the immune system(12). However, many new genes are being discovered that have roles in the autoimmune response in Crohn's disease and are giving more insight into how the disease operates and who is likely to contract it.
One gene, PTPN2, has recently been thought to have a close role with Crohn's. This gene is of particular interest because it is involved in mediating immune signaling through phosphorylation in the immune system. People and organisms with Crohn's often have mutations and differring protein expression of PTPN2.
One gene, PTPN2, has recently been thought to have a close role with Crohn's. This gene is of particular interest because it is involved in mediating immune signaling through phosphorylation in the immune system. People and organisms with Crohn's often have mutations and differring protein expression of PTPN2.
PTPN2 Gene
The PTPN2 gene on chromosome 18 encodes a tyrosine kinase
protein that regulates cytokine-induced signaling pathways, epithelial barrier
function, and cytokine secretion in the intestinal cells [8].
Disturbance in the PTPN2 gene causes impaired autophagosome formation, which leads to disruption of the immune system and contributes to the development of Crohn’s disease [9].
Studies identifying risk genes in people with Crohn's have found a significant link to PTPN2. The most notable research has been performed with mouse models of the disease where Crohn's phenotypes (like diarrhea and bloody stool) were observed in the mice after gene knockout of PTPN2(mouse model study). The mouse experiment demonstrates how dysfunction of PTPN2 leads to Crohn's disease, which makes PTPN2 a very vital piece to the puzzle of Crohn's disease.
Disturbance in the PTPN2 gene causes impaired autophagosome formation, which leads to disruption of the immune system and contributes to the development of Crohn’s disease [9].
Studies identifying risk genes in people with Crohn's have found a significant link to PTPN2. The most notable research has been performed with mouse models of the disease where Crohn's phenotypes (like diarrhea and bloody stool) were observed in the mice after gene knockout of PTPN2(mouse model study). The mouse experiment demonstrates how dysfunction of PTPN2 leads to Crohn's disease, which makes PTPN2 a very vital piece to the puzzle of Crohn's disease.
Treatment for Crohn's disease
There is no cure for Crohn’s disease, but there are ways to manage the disease in order to stay in remission and alleviate symptoms. Treatment varies patient to patient; types of treatment include anti-inflammatory drugs, immune system suppressors, nutrition therapy, antibiotics, and other medications used to control inflammation. In addition, surgery can be utilized as a last resort to remove a damaged part of the intestinal tract.
References
1. Lerebours E, Fower-Rousseau C, Merle V, et al. Stressful life events as a risk factor for inflammatory bowel disease onset: A population-based case-control study. Am J Gastroenterol 2007; 102: 122-31.
2. Kaplan GG, Hubbard J, Korzenik J, et al. The inflammatory bowel diseases and ambient air pollution: a novel association. Am J Gastroenterol 2010; 105: 2412-19
3. Hou JK, Abraham B, El-Serag H. Dietary intake and risk of developing inflammatory bowel disease: a systematic review of the literature. Am J Gastroenterol 2011; 106:563-73.
4. Seksik P, Nion-Larmurier I, Sokol H, Beaugerie L, Cosnes J. Effects of light smoking consumption on the clinical course of Crohn’s disease. Inflamm Bowel Dis 2009: 15: 734-41.
5. Jones DT, Osterman MT, Bewtra M, Lewis JD. Passive smoking and inflammatory bowel disease: a meta-analysis. Am J Gastroenterol 2008; 103: 2382-93.
6. Tuvlin JA, Raza SS, Bracamonte S, et al. Smoking and inflammatory bowel disease: trends in familial and sporadic cohorts. Inflamm Bowel Dis 2007; 13: 573-79.
7. Glas J, Wagner J, Seiderer J, et al. PTPN2 gene variants are associated with susceptibility to both Crohn’s disease and ulcerative colitis supporting a common genetic disease background. PLoS One 2012;7:3.
8.. Scharl M, Rogler G. The role for protein tyrosine phosphatase nonreceptor type 2 in regulating autophagosome formation. Ann N Y Acad Sci 2012; 1257: 93-102.
2. Kaplan GG, Hubbard J, Korzenik J, et al. The inflammatory bowel diseases and ambient air pollution: a novel association. Am J Gastroenterol 2010; 105: 2412-19
3. Hou JK, Abraham B, El-Serag H. Dietary intake and risk of developing inflammatory bowel disease: a systematic review of the literature. Am J Gastroenterol 2011; 106:563-73.
4. Seksik P, Nion-Larmurier I, Sokol H, Beaugerie L, Cosnes J. Effects of light smoking consumption on the clinical course of Crohn’s disease. Inflamm Bowel Dis 2009: 15: 734-41.
5. Jones DT, Osterman MT, Bewtra M, Lewis JD. Passive smoking and inflammatory bowel disease: a meta-analysis. Am J Gastroenterol 2008; 103: 2382-93.
6. Tuvlin JA, Raza SS, Bracamonte S, et al. Smoking and inflammatory bowel disease: trends in familial and sporadic cohorts. Inflamm Bowel Dis 2007; 13: 573-79.
7. Glas J, Wagner J, Seiderer J, et al. PTPN2 gene variants are associated with susceptibility to both Crohn’s disease and ulcerative colitis supporting a common genetic disease background. PLoS One 2012;7:3.
8.. Scharl M, Rogler G. The role for protein tyrosine phosphatase nonreceptor type 2 in regulating autophagosome formation. Ann N Y Acad Sci 2012; 1257: 93-102.
Specifications of PTPN2:
mRNA Accession #: NM_002828.3, FASTA
Protein Accession #: NP_002819.2, FASTA
Chromosome 18
mRNA Accession #: NM_002828.3, FASTA
Protein Accession #: NP_002819.2, FASTA
Chromosome 18
MAPS
|
|
|
Katherine Waldeck
[email protected]
Last Updated: 5/13/2015
University of Wisconsin-Madison
[email protected]
Last Updated: 5/13/2015
University of Wisconsin-Madison